The Daily Explains: Navigating COVID-19, monkeypox and the flu this season
Daily file illustration by Olivia Abeyta
Vaccines are currently available for all three viruses to increase immunity in case of exposure.
October 5, 2022
Wintertime may look bleak in Chicago, but your health and wellness don’t have to be. The public health landscape can often seem daunting, but The Daily is here to break down the three prevalent viruses to watch out for this season.
How an outbreak becomes an epidemic
Outbreaks can lead to epidemics or pandemics if case numbers rise quickly within a short period of time. These pandemics differ from seasonal variations in that people have little to no immunity given the novelty of the viruses.
On the other hand, the seasonal flu leads to an expected rise in cases that peaks between December and February. Scientists develop a new influenza vaccine yearly to target virus mutations and waning immunity over time, though previous infection and vaccination offer some immunity.
Though coronaviruses have also been around for a while, the COVID-19 pandemic originated from the SARS-CoV-2 strain. With mutations affecting the infectivity and severity of the disease, vaccine modifications have followed. Similarly to the seasonal flu, infections and booster doses strengthen immunity against COVID-19.
How each virus spreads
The key difference between the recent monkeypox outbreak, the seasonal flu and the COVID-19 pandemic is the rate at which transmission occurs.
Monkeypox primarily spreads through close, skin-to-skin contact, which can include direct contact to monkeypox rash or fluids from an infected person. The virus is therefore not as easily transmissible as COVID-19 and the flu, which primarily spread through respiratory droplets. Though the majority of monkeypox cases have been reported among men who have sex with other men, anyone who has close contact with an infected person can contract the virus.
COVID-19 and the flu spread in similar ways, but the smaller particle sizes of SARS-CoV-2 allow these respiratory droplets to stay in the air longer, increasing the rate of infection. This difference has made COVID-19 spread more rapidly than the flu.
COVID-19 also has a longer incubation period than the flu: someone who contracts the flu will typically experience symptoms within one to two days of exposure, while an individual with COVID-19 may not experience symptoms until within two days to two weeks. With this delay between symptom onset and viral exposure, people are more likely to spread SARS-CoV-2 before they quarantine or isolate.
Monkeypox has an even wider incubation period, ranging from five to 21 days.
Symptoms to watch out for
COVID-19 and the seasonal flu have many overlapping symptoms, including fever, fatigue, headache and nausea. However, unlike the flu, COVID-19 may also present with loss of taste or smell as well as shortness of breath.
Though monkeypox symptoms also include fever, headache and exhaustion, the more distinctive symptoms include rash and swollen lymph nodes. Symptoms typically persist for two to four weeks.
Prevention and possible treatment
Vaccines are currently available for all three viruses to increase immunity in case of exposure.
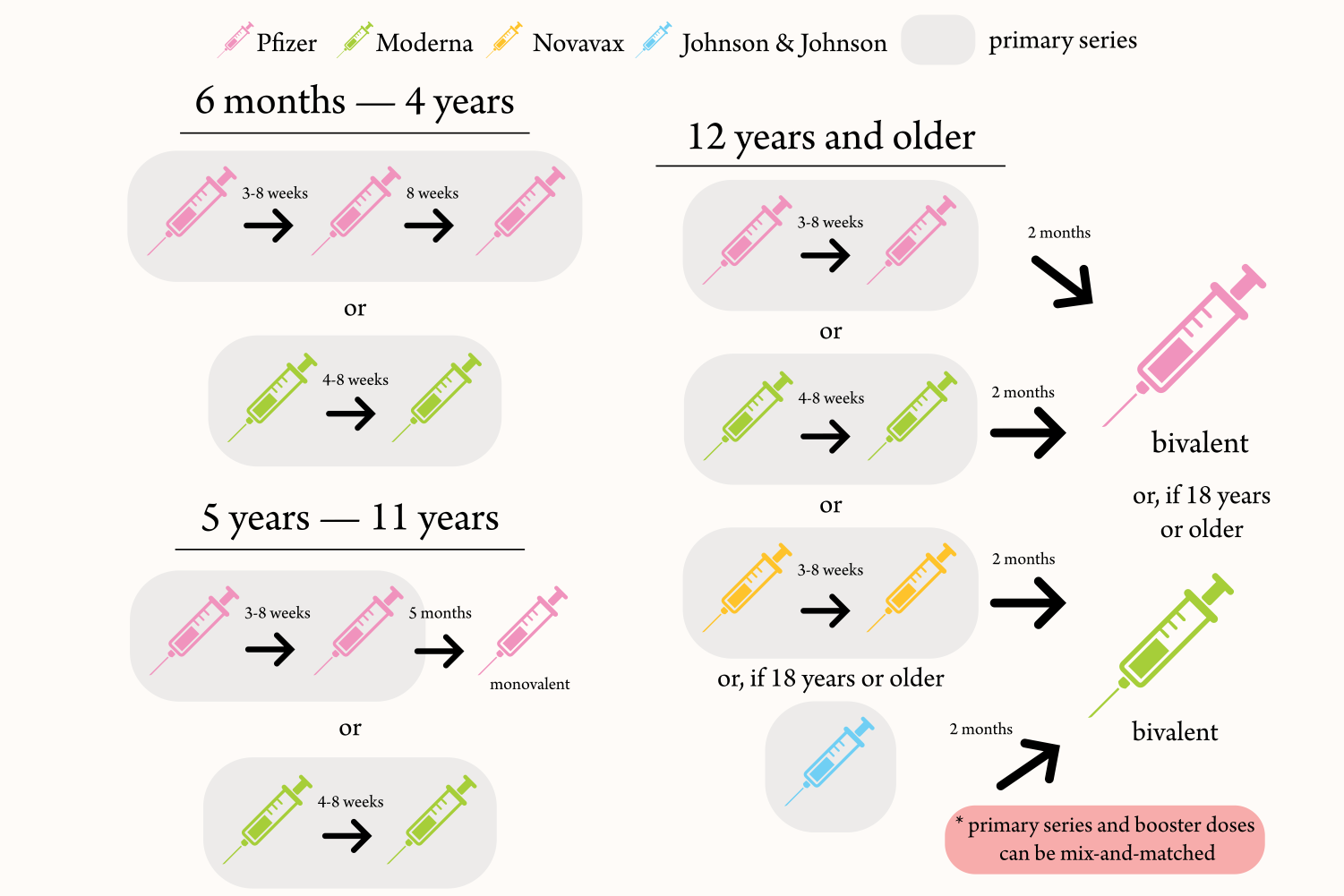
For COVID-19, vaccination eligibility differs by age. The Centers for Disease Control and Prevention recommend first receiving a two- or three-dose primary vaccination series of Pfizer, Moderna or Novavax, or the one-dose Johnson & Johnson vaccine.
Those 12 years or older should then receive a bivalent booster dose — authorized Sept. 1 — at least two months after their last COVID-19 vaccination. This updated dose provides protection against the original COVID-19 virus as well as the more infectious omicron BA.4 and BA.5 variants that comprise the majority of current infections.
Individuals between the ages of five and 11 are not yet eligible for the bivalent booster dose and should instead get the original monovalent booster dose at least five months after their last COVID-19 vaccination if they received the Pfizer primary-series vaccination.
The CDC has approved two vaccines for monkeypox, though vaccination is only recommended for those exposed to monkeypox or at high risk of exposure. Eligible individuals can either receive the two-dose Jynneos vaccination series or the single-dose ACAM2000 vaccine. Northwestern Medicine Student Health Service provides a list of local monkeypox vaccine providers on its website.
In terms of influenza vaccination, the CDC recommends individuals obtain the single-dose flu vaccine by the end of October. NU students can make a flu vaccine appointment at the Evanston campus, and all individuals can seek vaccination at nearby pharmacies like CVS and Walgreens.
In terms of treatment, a health care professional can prescribe antiviral medications for the influenza virus. For COVID-19 and monkeypox, professionals can prescribe antiviral medications to eligible, high-risk populations.
University policies and guidelines
NU currently does not have vaccination requirements for the flu or monkeypox but encourages vaccination against these viruses for eligible individuals. All community members are required to have at least primary-series vaccination unless granted an exemption.
Individuals who suspect they have monkeypox should contact the health service for assessment and treatment. Students who test positive are required to self-isolate until fully healed in order to prevent transmission of the virus — including using separate bathrooms, towels, clothing and linens from others. If living on campus, individuals must seek temporary off-campus housing for the duration of the isolation period, though the University has a limited number of isolation spaces available.
If students test positive for COVID-19, they will also be required to isolate for a minimum of five days. Students living on campus must complete their isolation period at 1835 Hinman Ave. NU recently updated its isolation housing policies for Fall Quarter.
While the University doesn’t have isolation requirements for the flu, the CDC recommends isolation protocols similar to those outlined for COVID-19. Infected individuals should self-isolate until at least 24 hours after the absence of fever without fever-reducing medications.
Email: [email protected]
Twitter: @amittal27
Related Stories:
— LTE: What you need to know about monkeypox
— NU COVID-19 isolation housing evolves, NU provides no booster shot update
— The Daily Explains: What you need to know about the flu season during COVID-19