For Northwestern Memorial Hospital workers on the front lines, vaccine brings morale boost, continued resolve
Courtesy of Northwestern Medicine Media Relations
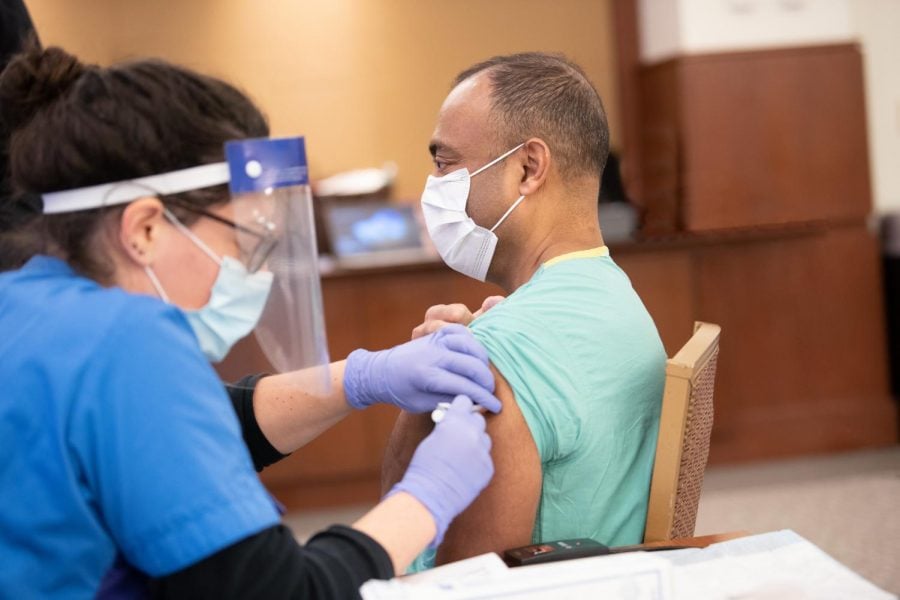
Ravi Fernando, a respiratory therapist at Northwestern Memorial Hospital, receives one dose of the vaccine. For Fernando and other healthcare professionals, the vaccine has provided a morale boost.
January 20, 2021
When Nancy Foster, a nurse manager for one of Northwestern Memorial Hospital’s COVID-19 units, received the first dose of the Pfizer-BioNTech COVID-19 vaccine on Dec. 18, a familiar face administered it.
That face belonged to Northwestern Memorial Hospital Education Coordinator Lizzy Murphy— an emotional sight, Foster said, because they had been through the pandemic together since it began. Of the 40 different stations Foster estimated were set up, Murphy’s happened to be the available one.
“I literally cried. Somebody took a picture and I sent it to my family,” said Foster, who received her second dose on Jan. 8. “And I’m like, ‘This is one step closer.’ So it was very, very emotional.”
For Northwestern Memorial Hospital healthcare professionals who have upended their personal lives to treat COVID-19 patients, the vaccine has provided a morale boost. There were tears and smiles around the hospital on the day the vaccinations arrived.
The vaccinations — created in record speed and using mRNA technology — have arrived after months of sacrifices made by people around the world, especially healthcare workers, who were among the first groups to receive it.
From April through August, Dr. Khalilah Gates averaged working one week on and one week off at the intensive care unit — “very much a lot of ICU time,” she said. Gates, a pulmonary and critical care specialist at Northwestern Memorial Hospital, now said she has about two weeks off between returns — time that will be spent teaching medical students and serving as assistant dean of undergraduate medical education at the Feinberg School of Medicine.
The added “layer of protection” from the vaccine has eased anxieties around whether her personal protective equipment would sufficiently shield her.
“I had to make a decision of do I accept the unknowns of the vaccine? Or do I accept the knowns and some of the unknowns of COVID? And the risk of accepting the unknown of the vaccine clearly outweighed COVID,” said Gates, who received her second dose on Jan. 8.
Ravi Fernando, a respiratory therapist at Northwestern Memorial Hospital, said he has been treating patients in the COVID-19 intensive care unit since February. From then until June 20, he said he didn’t return home, instead finding himself “stuck” in a hotel to avoid infecting his family.
Having received the second and final dose of the vaccine on Jan. 8, Fernando said it has brought peace of mind. While he experienced chills and a body ache after the last dose, he said an immune response isn’t abnormal. He felt fine the following morning.
“I feel like me and my family and people around me are protected,” Fernando said. “I highly recommend all my friends and everybody to take it if they have access to the vaccine.”
The vaccine has also brought a “huge sense of relief” for Dr. Marc Sala, a pulmonary and critical care specialist at Northwestern Memorial Hospital who has been splitting time between the ICU and a pulmonology clinic for long-haul COVID patients.
In the clinic, he said people of all ages and varying medical histories have entered with prolonged fatigue, shortness of breath, cough and “brain fog.” In the ICU, he has performed bronchoscopies and other procedures that could entail significant viral load exposure.
For over nine months now, Sala described a sense of stress associated with not knowing if he would be next among his colleagues or the general public to wind up in an ICU bed. Additional conversations with his wife, also a physician, about living wills and estate plans were “a lot emotionally,” Sala said.
“And then you go to work and if you get exposed to some of the virus… That’s a whole different acute stress because now you have to isolate, you have to either live somewhere else or isolate within your own home. You can’t hug and kiss your kids or your spouse. And you just are on needles until you get that test result and can take your mask off in your own house,” Sala said. “And that’s just independent of the fact that ICU care is an extraordinarily intense atmosphere.”
In addition to personal relief, the vaccine has also brought hope for healthcare professionals that there is an end in sight to this pandemic. But they caution against taking personal vaccination as an excuse to return to pre-pandemic ways of life.
Fernando noted that the Pfizer-BioNTech COVID-19 vaccine is 95 percent efficacious, meaning there is still a five percent chance he could contract the virus. Until the entire country reaches herd immunity, he emphasized the need for compliance with guidelines from the Centers for Disease Control and Prevention.
Another caveat to the Pfizer-BioNTech COVID-19 vaccine, Sala said, is that the existing data does not show whether a vaccinated person could still spread the infection asymptomatically.
“The wrong thing to do, medically speaking, is to let your guard down to think that you couldn’t be a carrier or affect harm to other people by spreading it,” Sala said.
The vaccine’s arrival has been stymied by the emergence of new strains, some believed by scientists to be more contagious, making vaccine rollout all the more important.
While this is a moment of hope for healthcare providers, Gates said it must also be one of education.
“I am very frank with my patients. There is no pressure, but there is education. So let’s talk about it: What are your concerns? Why are you saying right off the bat you know you’re not going to do it?” Gates said. “Let’s talk about the data that shows (the vaccine) is safe, at least in the short term.”
As an African American doctor, Gates said she tries to answer questions from more vulnerable communities and has a Q&A about the vaccine planned with one of the Chicago Public Schools.
Fernando stressed the need to calm fears from people of color, who he said disproportionately make up the majority of his sickest patients.
“I’m South Asian. I’m a brown dude. So especially I have an understanding that people (of) color… they have a really big fear to take the vaccine,” Fernando said. “We need to convince them more. They are more vulnerable to the disease.”
Email: [email protected]
Twitter: @pamesjollard
Related stories:
— Northwestern doctors upend family life to fight at frontlines, NM builds capacity for peak
— Northwestern doctors face challenges in psychiatric care, anticipate mental health crisis ahead