NU researchers develop wearable throat sensor to help stroke patients
Source: Elliott Abel/Shirley Ryan AbilityLab
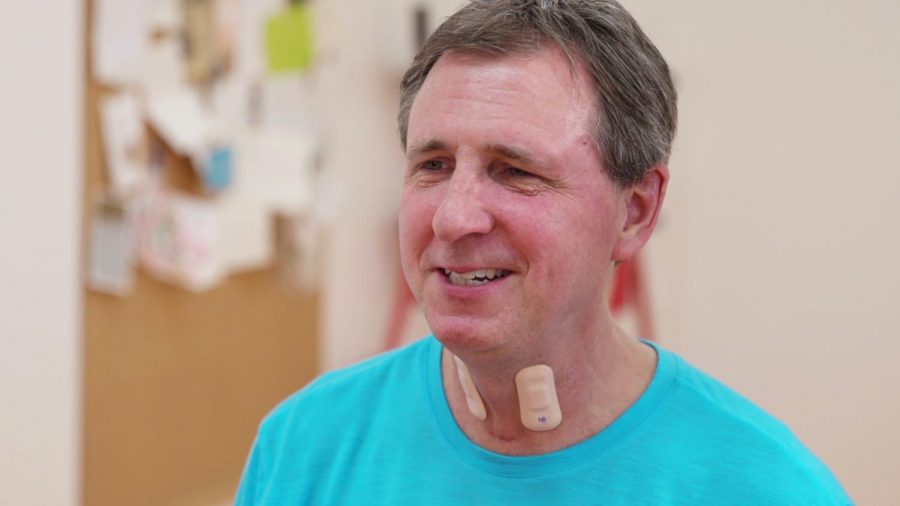
A man wears throat sensors designed by McCormick and Feinberg Prof. John Rogers’ lab, in partnership with the Shirley Ryan AbilityLab.
February 22, 2018
Northwestern researchers partnering with a research hospital in Chicago have developed a wearable throat sensor that could help patients undergoing rehabilitation after stroke.
According to a Feb. 17 news release, McCormick and Feinberg Prof. John Rogers’ lab, in partnership with the Shirley Ryan AbilityLab, developed a stretchable electronic sensor that helps diagnose and treat patients with aphasia — a speech impediment that can result from stroke. The sensor may help facilitate the recovery process of stroke patients even after they are discharged from the hospital.
Tools traditionally used by speech-language pathologists — who diagnose and treat speech and language problems — cannot distinguish between patients’ voices and background noise, according to the release.
“Our sensors solve that problem by measuring vibrations of the vocal cords,” Rogers said in the release. “But they only work when worn directly on the throat, which is a very sensitive area of the skin. We developed novel materials for this sensor that bend and stretch with the body, minimizing discomfort to patients.”
According to the release, the throat sensor measures patients’ swallowing ability and patterns of speech.
Rogers told The Daily that the throat sensor lasts 12 hours and is meant to be worn throughout the day. The device can be recharged while a patient is asleep, which is when monitoring speech is not as important, he said.
Feinberg Prof. Arun Jayaraman, who is a research scientist at the Shirley Ryan AbilityLab, told The Daily that the throat sensor is among several sensors created to help stroke patients, including some designed to monitor movement and cardiac behavior.
Multiple sensors can be placed on different parts of the body to capture a detailed, “full-body assessment of one’s physiological health,” Rogers told The Daily, adding that his lab has been working with the AbilityLab to develop sensors that track a patient’s status as they go through rehabilitation.
“Being able to quantify those things allows the physicians for the first time to measure in a detailed way the condition of a patient at any time as they progress through their course of rehabilitation,” Rogers said. “(That allows them to) tailor on an individual basis the rehabilitation protocol.”
Jayaraman told The Daily that the sensors, which enable doctors and clinicians to keep an eye on the patients after they have been discharged from the hospital, will help provide individualized care for patients on a more real-time basis. The devices may help expedite patients’ recovery process, he added.
Patients receive “pretty intensive” rehabilitation in the hospital, but tend to lose some of that progress — such as in speech, swallowing and walking — after they leave, Jayaraman said. He added that the devices will help doctors monitor compliance and intervene if they see a “certain significant drop off.”
The devices can be worn without affecting daily activities, Rogers said, and conform to the curves of the body. He added that information from the sensors is “continuously streaming in a wireless mode.”
Jayaraman said Rogers developed the “hardware” for the sensors, while the AbilityLab takes the data from the sensors and creates specific algorithms to monitor specific impairments.
“You don’t even realize that the device is on your body after you’ve put it on,” Rogers said. “Think about (the device) as a thin Band-Aid but with full electronic capability in the sense of batteries for power supplies, radios for wireless data communication (and) an entire suite of sensors that capture clinical-quality data.”
Email: [email protected]
Twitter: @thisisalane